In the world of diet fads and health trends, the topic of gluten-free diets often dominates. The gluten-free diet gained popularity due to claims of weight loss, improved digestion, increased energy, and clearer skin. Media attention from books, diet “experts,” and celebrities serve to promote these claims, leaving many to wonder whether they should remove gluten from their diets. In this month’s Fueling Facts, our nutrition team explains what gluten is, when it may make sense to adopt a gluten-free diet, and how gluten-containing foods can actually benefit the body.
What is gluten?
Gluten is a protein found in wheat, rye, and barley. It is considered a prolamin, meaning it is rich in proline and glutamine (two amino acids, which are building blocks of proteins). Gluten acts as a binding agent and provides elasticity to pastas, breads, and pastries. Because of its binding properties, gluten is also found in a variety of foods unexpectedly, including salad dressings, soy sauce, ice creams, seasoning mixes, vinegars, and French fries.1,2 With the rise in popularity of gluten-free diets, the food industry now produces a vast selection of gluten-free products. However, when gluten is removed from a product or recipe, the remaining ingredients often become dry and brittle, which makes it necessary to add a replacement binding agent, such as eggs, xanthan gum, or guar gum. For this reason, many processed gluten-free products replace essential nutrients with added ingredients, such as sugars, resulting in a less nutrient-dense product compared to conventional gluten-containing foods.
How does the body digest gluten?
Most people digest foods containing gluten without issue. The digestion process begins in the stomach when pepsin, an enzyme, begins the breakdown of gluten into peptides. From there, it moves into the small intestine, where other enzymes, including protease, chymotrypsin, elastase, and carboxypeptidase, breakdown the gluten into even smaller peptides. In the small intestine the villi (finger-like projections along the intestinal wall) absorb amino acids and transport them into the bloodstream for use by various tissues.1
Who should avoid gluten?
While most individuals can eat and digest without issue, gluten-free diets are indicated for those with celiac disease, a wheat allergy, non-celiac gluten sensitivity, or other autoimmune conditions.
Celiac Disease
About 1% of the Western world suffers from celiac disease, a chronic, gastrointestinal, immune-mediated disease triggered by exposure to gluten proteins. Most cases are diagnosed in childhood, but CD can develop at any age due to genetic and environmental factors.2 Symptoms of CD range from mild to severe, but tend to include diarrhea, bloating, skin rashes, nausea, and constipation. A diagnosis requires the presence of villi atrophy (i.e., degeneration) as shown from a small intestinal biopsy taken via endoscopy and a positive serologic test for immunoglobin A (IgA). To protect against false negatives for those with an IgA deficiency, immunoglobin G (IgG) is a secondary biomarker for CD diagnosis.3 Susceptibility to CD is strongly associated (i.e., 90% of CD patients have one or both genes) with the human leukocyte antigen (HLA) genes, DQ2 and/or DQ8.1 While ~30% of the population carries a genetic predisposition for CD, only ~3% will develop the disease.
When people with CD consume gluten, the prolamins (high concentrations of proline and glutamine) trigger an autoimmune response in the small intestine. The antibody cells attack and cause damage to the villi along the intestinal wall, causing the villi’s structure to flatten (see image below). This structural change reduces the surface area for nutrient absorption, potentially leading to nutrient deficiencies if the inflammation is not resolved (i.e., the trigger, gluten, continues to be consumed). Long-term effects of poorly controlled CD include: osteoporosis, infertility, and neurological impairments.1 The primary treatment available for those with celiac disease is a strict gluten-free diet, which must be followed for life to prevent intestinal damage and poor health outcomes.

Wheat Allergy
Individuals with wheat allergies can experience an immune- or nonimmune-mediated response following the consumption of wheat-containing foods, such as breads, pastas, cereals, and crackers. Individuals can develop an allergy to any of the four classes of wheat proteins – albumin, gliadin, globulin, and of course, gluten. While gluten is the only protein that needs to be eliminated for someone with CD, all wheat products must be eliminated for someone with a wheat allergy. However, those with a wheat allergy can most likely consume other grains, such as barley, rye, and oat, if the allergy is not of the gluten variety. Wheat allergies are diagnosed using skin-prick or blood tests.4
Non-Celiac Gluten Sensitivity (NCGS)
Some people consume gluten and experience gastrointestinal discomfort, such as significant bloating, constipation, nausea, gas, and diarrhea. If this occurs without the elevation of antibodies (unlike in those with CD or a wheat allergy), it is often referred to as non-celiac gluten sensitivity (NCGS). This is different from CD because those with NCGS can digest gluten without damaging the villi and therefore nutrient absorption is protected. Because there are no validated biomarkers for NCGS, diagnosis is difficult to identify. At-home food sensitivity tests are not recommended to explore the presence of a NCGS. Instead, your physician or dietitian may suggest a placebo-controlled gluten challenge or a food-symptom diary to explore the correlation between GI symptoms and gluten consumption. If diagnosed with NCGS, a dietitian can offer guidance on how to approach a gluten-free or gluten-limiting diet.4
Other Autoimmune Conditions
Those with existing autoimmune diseases, such as Type I diabetes, Hashimoto’s disease, Graves’ disease, or Addison’s disease are at higher risk of developing CD. In such cases, a physician may recommend a gluten-free diet depending on symptom presentation and disease pathology.4
A Note on Gluten-Free Eating
For those adhering to a gluten-free diet it is necessary to avoid not only wheat, but also rye, barley, and oats. Oats do not naturally contain gluten but are often cross-contaminated as they are regularly grown and processed near gluten-containing grains. It is also recommended to prioritize whole forms of gluten-free sources, such as corn, quinoa, amaranth, rice, buckwheat, and millet, as opposed to processed gluten-free substitutes. These whole food sources are higher in micronutrients and fiber and lower in added salt, sugar, and fat compared to their processed counterparts.
What are the benefits of gluten-containing whole grains?
Gluten-containing foods, particularly whole grain versions, are rich in fiber and micronutrients. Dietary fiber promotes a healthy intestine microbiome by serving as prebiotic “food” for the trillions of microorganisms inside the intestines. These microorganisms improve nutrient metabolism, protect against infection, and create beneficial byproducts (check out our previous blog post, Gut Microbiome: The Basics, for more information about fiber). Fiber also increases stool bulk, slows absorption of carbohydrates, and binds harmful LDL cholesterol in the intestines, resulting in decreased risk of diabetes and cardiovascular disease.6,7 During the process of creating a gluten-free substitute, fiber is typically lost in the production. For example, when comparing fiber content of whole grain and gluten-free bread, Dave’s Killer Bread® (whole grain) contains 4 more grams of fiber than the Udi’s® gluten-free substitute. The essential micronutrients within gluten-containing grains, such as iron, magnesium, zinc, folate, and phenolic acids, also contribute important health benefits.
- Iron transports oxygen in our blood.8
- Magnesium improves bone health, neurological function, and muscle contraction.9
- Zinc has anti-inflammatory, wound healing, and immunity-building properties.10
- Folate, also known as vitamin B9, aids in red blood cell formation, DNA and RNA synthesis, and protein metabolism.11
- Phenolic acids act as powerful antioxidants within the body that lower risk of cancer and many chronic diseases.12
These nutrients are typically lost in the process of creating a gluten-free substitute, leaving behind a nutrient-poor product.4 Not only do gluten-free substitutes contain less micronutrients, but they also often include added sugars, salt, and fats to compensate for gluten’s effects on food texture and mouthfeel. In fact, a 2021 study reviewed over three thousand gluten-free products and showed no nutritional advantage of gluten-free products when compared to their gluten-containing counterpart.4
Some individuals question whether gluten belongs in a healthy diet due to negative media attention. These claims remain unsubstantiated and, in fact, published research confirms the opposite.4 Epidemiological studies show that the incorporation of whole grains as a part of a healthy diet plays a role in reducing cardiovascular disease, obesity, type 2 diabetes, and cancer risk. In short, cutting out gluten from your diet also means cutting out nutrient-dense whole grains and their related health benefits.
The Bottom Line
Gluten is a protein found in wheat, rye, and barley products that is safely consumed by most people. Although the gluten-free product industry continues to grow, evidence does not support the efficacy of following a gluten-free diet for those without medical indication and doing so could put you at risk for nutritional deficits.4,13 Instead, research supports including whole grains as a key component of a balanced diet due to the many benefits they provide. In fact, including whole grains are considered complex carbohydrates, which compose one quarter of a recommended Balanced Plate (see below).
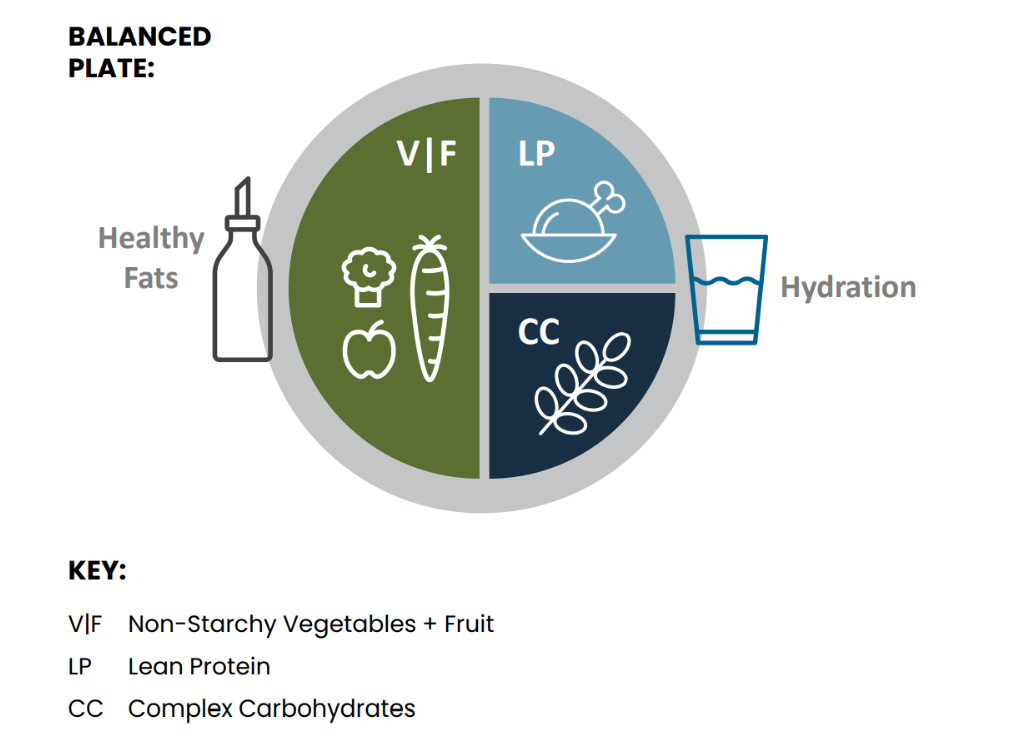
If you do not have celiac disease, a wheat allergy, or gluten sensitivity, consider these easy ways to incorporate more whole grains into your diet:
- Amp up your granola. Mix in wheat bran cereal, such as All Bran Buds®, to your favorite granola for a higher fiber topping to your yogurt.
- Choose nutrient-dense bread. Swap out a white bread for a high-fiber, whole-wheat variety like Dave’s Killer Bread® or Food for Life® Ezekiel.
- Start small. If your current grain intake is primarily white grains, try replacing half of the portion with a whole-wheat alternative.
If you have questions about gluten or how to incorporate more whole grains into your diet, please reach out to your SHIFT Registered Dietitian for individualized recommendations.
In Real Health,
Stephanie Schnaufer
SHIFT Dietetic Intern
References
- Haseeb M, Posner EB. Celiac disease – statpearls – NCBI bookshelf. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK441900/. Published August 2022. Accessed April 10, 2023.
- Fernández-Pérez S, Pérez-Andrés J, Gutiérrez S, et al. The Human Digestive Tract Is Capable of Degrading Gluten from Birth. Int J Mol Sci. 2020;21(20):7696. Published 2020 Oct 18. doi:10.3390/ijms21207696
- Celiac disease tests – NIDDK (no date) National Institute of Diabetes and Digestive and Kidney Diseases. U.S. Department of Health and Human Services. Available at: https://www.niddk.nih.gov/health-information/professionals/clinical-tools-patient-management/digestive-diseases/celiac-disease-health-care-professionals (Accessed: April 20, 2023).
- Cárdenas-Torres FI, Cabrera-Chávez F, Figueroa-Salcido OG, Ontiveros N. Non-Celiac Gluten Sensitivity: An Update. Medicina (Kaunas). 2021;57(6):526. Published 2021 May 24. doi:10.3390/medicina57060526
- Lauret E, Rodrigo L. Celiac disease and autoimmune-associated conditions. Biomed Res Int. 2013;2013:127589. doi:10.1155/2013/127589
- Niland B, Cash BD. Health Benefits and Adverse Effects of a Gluten-Free Diet in Non-Celiac Disease Patients. Gastroenterol Hepatol (N Y). 2018;14(2):82-91.
- Ioniță-Mîndrican CB, Ziani K, Mititelu M, et al. Therapeutic Benefits and Dietary Restrictions of Fiber Intake: A State of the Art Review. Nutrients. 2022;14(13):2641. Published 2022 Jun 26. doi:10.3390/nu14132641
- Xu D, Fu L, Pan D, et al. Role of whole grain consumption in glycaemic control of diabetic patients: A systematic review and meta-analysis of randomized controlled trials. Nutrients. 2021;14(1):109. doi:10.3390/nu14010109
- Moustarah F, Daley SF. National Center for Biotechnology Information. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK540969/. Published October 22, 2022. Accessed April 14, 2023.
- Al Alawi AM, Majoni SW, Falhammar H. Magnesium and Human Health: Perspectives and Research Directions. Int J Endocrinol. 2018;2018:9041694. Published 2018 Apr 16. doi:10.1155/2018/9041694
- Saper RB, Rash R. Zinc: an essential micronutrient. Am Fam Physician. 2009;79(9):768-772.
- Office of dietary supplements – folate. NIH Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/. Published November 30, 2022. Accessed April 14, 2023.
- Diez-Sampedro A, Olenick M, Maltseva T, Flowers M. A Gluten-Free Diet, Not an Appropriate Choice without a Medical Diagnosis
- Khan J, Khan MZ, Ma Y, et al. Overview of the Composition of Whole Grains’ Phenolic Acids and Dietary Fibre and Their Effect on Chronic Non-Communicable Diseases. Int J Environ Res Public Health. 2022;19(5):3042. Published 2022 Mar 5. doi:10.3390/ijerph19053042
- . J Nutr Metab. 2019;2019:2438934. Published 2019 Jul 1. doi:10.1155/2019/2438934
